Sandy McLachlan
Clinical history
Query enterotoxigenic E.coli, torsion, sepsis? Metronidazole had been administered by the owner in the morning. Late afternoon the dog presented to the attending veterinarian with fever 40.9°C, and was treated with cefazolin, enrofloxacin, IV fluids, meloxicam and maropitant. In house CBC showed haemoconcentration (HCT 69.5% (37.3 – 61.7)) and profound leukopenia (neutrophils 0.04 x 109/L (2.95 – 11.64), lymphocytes 0.24 x 109/L (1.05 – 5.10)). An in-house faecal snap test was negative for coronavirus, parvovirus and Giardia. The dog was euthanised the following morning.
Gross postmortem examination findings
The body was in rigor (4 ½ hours after euthanasia). The tongue was deep purple (cyanotic). The subcutis lacked elasticity. A skin tent could be made with difficulty and then remained for >30 seconds (dehydration). There was no subcutaneous, abdominal, perirenal, pericardial or bone marrow fat (emaciated). There were petechial haemorrhages throughout the subcutis. There was generalised vascular congestion of all tissues.
The thymus was severely congested. The thorax was 1/3 full of clear serosanguinous fluid. The pericardial sac was distended by clear straw-coloured fluid with a strand of fibrin at the heart base [swab taken]. The heart was large (athletic hypertrophy). There were many subepicardial ecchymotic haemorrhages around the heart base and on the atria. There were a few subendocardial ecchymotic haemorrhages in the ventricles at the origin of the chordae tendinae.
The lungs were not collapsed, and the lung parenchyma was dark red and had a jelly-like consistency. Bloody fluid oozed from the cut surface of the lung parenchyma. The trachea was full of foam to the level of the larynx. The abdomen was half full of turbid serosanguinous fluid. There were petechial haemorrhages scattered throughout the serosa.
The stomach was half full of watery fluid [approximately 300 mL]. At the junction of the pylorus of the stomach and proximal duodenum were six ulcers in the mucosa that were 3 to 5 mm diameter and did not perforate through the pyloric wall. The intestines were empty except for mucus and bile.
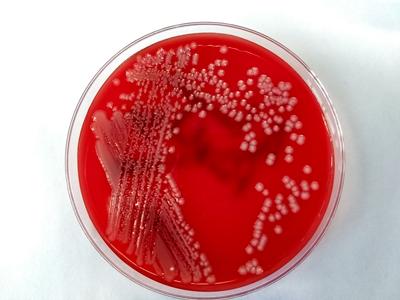
Bacteriology
Heart (epicardium) swab: heavy growth of Acinetobacter baumannii. Lung: heavy growth of A. baumannii.
The gross post-mortem examination findings together with culture of a heavy pure growth of A. baumannii from lung and the epicardium are consistent with pneumonia and systemic disseminated intravascular coagulation and fibrinolysis.
Histopathology
The most striking histologic findings were in the lung, oesophagus, and gastro-duodenal junction.
In the lung the lumen of bronchioles and the surrounding alveoli were filled with degenerate neutrophils and sero-fibrinous exudate. Many of the degenerate neutrophils had phagocytosed coco-bacilli in the cytoplasm. The coco-bacilli stained Gram-negative.
The stratified squamous epithelium of the oesophagus was lost leaving only a few scattered remnants. The surface of the exposed lamina propria comprised a grey coagulum.
At the stomach pylorus – duodenum junction there were ulcers in the mucosa 2 – 4 mm wide that extended through the muscularis mucosa to the submucosa. In the ulcer bed the exposed surface of the submucosa
Microscopic morphologic diagnoses
· Lung: acute fulminant suppurative bronchopneumonia with intra-lesional coco-bacilli (inhalation pneumonia).
· Oesophagus: mucosal ulceration.
· Stomach pylorus / duodenum junction: multifocal mucosal ulcers.
Summary
The histologic findings corroborated the gross findings. There was acute fulminant bronchopneumonia associated with an overwhelming infection with A. baumanii followed by septic (endotoxic) shock.
Ulceration of the oesophagus is an unusual finding. A possible cause of oesophageal ulceration is repeated regurgitation or vomiting of stomach acid. Regurgitation or vomiting may be associated with stomach ulcers and are factors for inhalation bronchopneumonia.
A. baumannii is an emerging opportunistic bacterium associated with Gram-negative sepsis, most frequently acquired as a nosocomial infection. It was nicknamed Iraqibacter because it first rose to prominence in military hospitals during the Iraq war.
A. baumanii is frequently resistant to antimicrobials. In this case the bacterium was sensitive to enrofloxacin, tetracycline, sulpha/trimethoprim, and gentamicin, but resistant to cephalothin, amoxicillin/
clavulanic acid, ampicillin and
cefazolin.
